Your cart is currently empty!
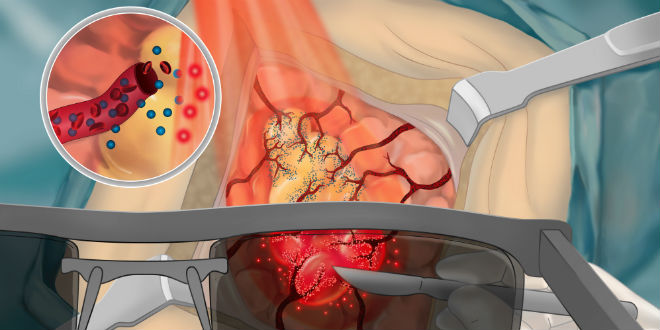
Israeli ‘Smart Probe’ That Excels at Detecting Cancer Cells May Improve Survival Rates
Many cancer patients die not from the localized malignant tumor that is removed in surgery but when lingering cancer cells from the tumor spread by metastasis. Now, a team of researchers headed by Prof. Ronit Satchi-Fainaro of the physiology and pharmacology department of at Tel Aviv University’s Sackler Faculty of Medicine believe they have found a way to rein in these bandit cells that could dramatically improve the chances for patients after surgery.
They developed a fluorescent tag of injected polymers that is activated by an enzyme of which the cancer cells produce too much. This smart “Turn-ON” probe for guided imaging surgery is injected into the oncology patient a few hours before an operation to remove the primary tumor. The tag helps the surgeons pinpoint exactly where the cancer – even just a few cells that can’t be identified with an magnetic resonance imaging (MRI) or computerized tomography (CT) scanner – is located. The doctors then can try to remove more cancer cells than was ever possible before.
“In cases of melanoma [the most dangerous skin cancer] and breast cancer, for example, surgeons may think they have removed everything and that the
patient is cancer free. But even if only a few cells remain after surgery, the cancer may recur and spread,” said Satchi-Fainaro, who is president of the Israeli
chapter of the Controlled Release Society and co-editor-in-chief of the journal Clinical Cancer Drugs. “Our new technology can guide the surgeon to
completely excise the cancer.”
The team, which included lab students Rachel Blau, Yana Epshtein and Evgeni Pisarevsky, has just published the discovery in the journal Theranostics .
“When the cyanine molecules are held together by the polymer particle, the light waves they emit cancel each other out, and they remain dark,” said Sachi-Fainaru. “But once the nanoparticle reaches a cancerous cell, the connecting polymer is cut. The cyanine molecules move away from each other and shine brightly, but in the surrounding healthy tissue the polymer is not cut, and the area remains dark. Cathepsin cuts the tag from the polymer and turns on its fluorescence at a near-infrared light, guiding the surgeon in real time while taking out the solid tumor so he or she can also avoid cutting out any “non-glowing” healthy tissue.
The TAU technique makes use of near-infrared technology to find proliferating cancer cells. “The probe is a polymer that connects to a fluorescent tag made of molecules of cyanine dye using a ‘linker,’ which is recognized by an enzyme called cathepsin. This substance is overproduced in many cancer types,” she explained.
In professional terms, it means that the smart sensor has high sensitivity (it detects all the cancer cells) and also high selectivity (it does not tag healthy cells). In this way, the surgeon identifies the location of the cancer cells in real time, that is, during the surgery itself. Existing imaging device cannot do this.
The scientists first examined the effect of the probe in the lab on healthy skin and mammary tissue, followed by melanoma and breast cancer cells. They then used mouse models of melanoma and breast cancer to perform routine tumor-removal surgeries and smart probe-guided surgeries.
“The mice that had regular surgery experienced recurrence and metastasis much sooner and more often than those that underwent our smart probe-guided surgery,” noted Satchi-Fainaro. “Most importantly, those which experienced the smart-probe surgery survived much longer.”

The results were very promising: mice analyzed without the sensor were soon diagnosed with metastasis or recurrence of the tumors themselves, and their life expectancy was short; only 40% of the mice in this group survived 120 days after the operation. But when the operation was performed using the new sensor, 80% of them remained healthy after 120 days. Thus, 60% of the mice analyzed the conventional way eventually died from the disease, compared to only 20% of those analyzed using the smart sensor.
The TAU scientist added that the probe may also cut the need for repeated surgeries in patients with cancer cells that remain in the edges of removed tissue. “Altogether, this can lead to the improvement of patient survival rates. We are currently designing and developing additional unique polymeric ‘Turn-ON’ probes for using in image-guided surgery. We are always looking for ways to improve sensitivity and selectivity, which are paramount to cancer patients’ care,” she concluded.
“We have registered several patents, concluded Sachi-Fainaru, “and now we are negotiating with a number of pharmaceutical companies to advance to clinical trials and later to commercial production that can significantly increase patients’ chances of surviving the disease.”
The post Israeli ‘Smart Probe’ That Excels at Detecting Cancer Cells May Improve Survival Rates appeared first on Breaking Israel News | Latest News. Biblical Perspective..
Source: Israel in the News
